Although gastroesophageal reflux disease (GERD) is a common condition and well known among the public, not only the recognition of its signs and symptoms should be emphasized, but also the pathophysiology – how it occurs – its treatment, and also the complications that can possibly bring about if GERD is not being managed properly. We have discussed about the above-mentioned topics about GERD, now let us focus on what are the available treatments to manage GERD. Also, there are important complications that should be noted so that the public can be aware of them and seek medical treatment as soon as possible once signs and symptoms of GERD are recognized.
Treatment
First and foremost, patients who face problem with GERD are advised to practice certain lifestyle modifications in order to prevent further damage to the esophagus and throat, as well as the ear especially in children.
Lifestyle Modifications
- Sleep with head elevated to about 15 to 20cm – this prevents the force of gravity from causing gastric content to flow back into the esophagus while sleeping. In symptomatic young children, avoid feeding them lying down, e.g. bottling them while the lie down

- Avoid eating before sleep – it is advised that one should not consume any food at least 2 hours before bedtime.
 Avoid beverages and food that can increase GERD symptoms –these include: coffee, tea (anything that contains caffeine), orange or lemon juices, spicy food, alcohol, etc.
Avoid beverages and food that can increase GERD symptoms –these include: coffee, tea (anything that contains caffeine), orange or lemon juices, spicy food, alcohol, etc.- Stop smoking – substances from cigarettes inhaled irritates the lining in the throat. Try to stop smoking to eliminate another cause of inflammation.

What are the medical treatments available to treat GERD?
There are over-the-counter drugs that are in the market to help improve symptoms of heartburn. Having said, it is best to seek medical advice from a physician about the specific signs and symptoms you are facing so that you can be prescribed the most suitable medications for optimal healing.
Antacids
Antacids are neutralizing agents that neutralize the acidity produced by the gastric juice. It acts by counteracting the low pH of acidity produced by the stomach. These are sold in pharmacy or health-care stores without the need of a doctor’s prescription. E.g: aluminium carbonate, magnesium hydroxide.
H2-receptor antagonists
 These helps to reduce histamine production by the stomach – specifically, they are produced by the parietal cells – thereby decreasing gastric acid secretion. E.g: ranitidine, cimetidine, famotidine.
These helps to reduce histamine production by the stomach – specifically, they are produced by the parietal cells – thereby decreasing gastric acid secretion. E.g: ranitidine, cimetidine, famotidine.
Proton-pump inhibitors (PPI)

PPI is a more potent anti-reflux agent although the target cells are also the parietal cells in the stomach – since the parietal cells are the main cells that are responsible in producing acid secretions. PPI directly and irreversibly blocks the enzyme that is involved in producing hydrogen ions (H+), i.e. acid, thus reducing the acid content in the stomach. E.g: omeprazole, esomeprazole, lansoprazole.
Prokinetic agents
 This class of drug helps to increase gastric emptying, which means, it is useful to quicken digestion. Hence, reduce time of food particles to stay in the stomach causing continuous acid production. E.g: metochlopromide, domperidone. They also help prevent nausea, vomiting and sense of bloatedness.
This class of drug helps to increase gastric emptying, which means, it is useful to quicken digestion. Hence, reduce time of food particles to stay in the stomach causing continuous acid production. E.g: metochlopromide, domperidone. They also help prevent nausea, vomiting and sense of bloatedness.
What if medications don’t work on me?
Then surgery would be advisable. Surgical options can also help to reduce the need of long-term medications.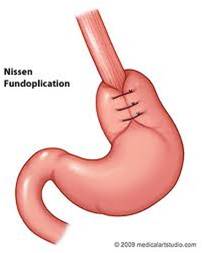
Nissen fundoplication
This is the standard surgical technique in treating GERD. The objective of this surgical technique is to reinforce and tighten the lower esophageal sphincter in order to prevent reflux. This is done by wrapping the very top of the stomach around the outside of the lower esophagus.
EndoCinch endoluminal gastroplication
This procedure uses the combination of the weakened lower esophageal sphincter and sutures to create a barrier in order to prevent the backup of stomach acid.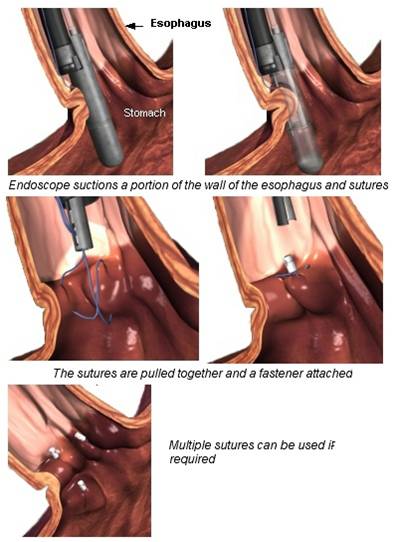
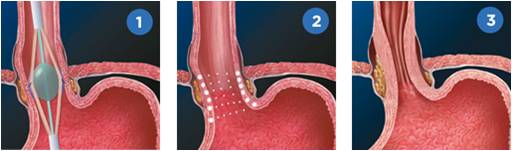
Stretta
Aside from using heat to form scar tissue in the lower esophagus via electrode energy, Stretta procedure also damages the nerve tissues that respond to reflux. The scar tissue that forms as the esophagus heals helps strengthen the muscles of the lower esophageal sphincter.
 EndoCinch and Stretta are new surgical techniques that are still under research about which candidate is suitable for these two procedures.
EndoCinch and Stretta are new surgical techniques that are still under research about which candidate is suitable for these two procedures.
Complications
Barrett’s esophagus
Barrett’s esophagus is a precancerous state of the esophagus, i.e. it has malignant potential to undergo cellular changes into esophageal cancer. Hence, making Barrett’s esophagus the most severe complication of GERD. Cellular changes of the lower part of the esophageal lining in Barrett’s esophagus are associated with increased risk of esophageal cancer. Approximately 15% of GERD patient are found to have Barrett’s esophagus. Doctors would perform surveillance endoscopy to watch out for early signs of esophageal adenocarcinoma.
Esophageal stricture
When inflammation of the esophagus due to acid reflux is not controlled or managed, deep scarring tissue forms, i.e. esophageal stricture. This is a narrowed pathway in the distal part of the esophagus causing difficulty in swallowing as food cannot pass through the thickened scarred tissue that is formed by the chronic and advanced stage of esophagitis.
