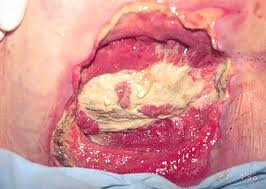
Aggravating the situation may be other conditions such as excess moisture from incontinence, perspiration or exudate. Over time, this excess moisture may cause the bonds between epithelial cells to weaken thus resulting in the maceration of the epidermis. Temperature is also a very important factor. The cutaneous metabolic demand rises by 13% for every 1°C rise in cutaneous temperature. When supply can’t meet demand, necrosis therefore occurs. Other factors in the development of bedsores include age, nutrition, vascular disease, diabetes mellitus, and smoking, amongst others.
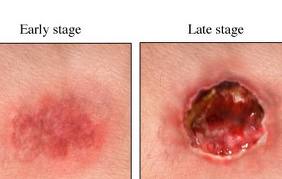 There are currently two major theories about the development of pressure ulcers. The first and most accepted is the deep tissue injury theory which claims that the ulcers begin at the deepest level, around the bone, and move outward until they reach the epidermis. The second, less popular theory is the top-to-bottom model which says that skin first begins to deteriorate at the surface and then proceeds inward.
There are currently two major theories about the development of pressure ulcers. The first and most accepted is the deep tissue injury theory which claims that the ulcers begin at the deepest level, around the bone, and move outward until they reach the epidermis. The second, less popular theory is the top-to-bottom model which says that skin first begins to deteriorate at the surface and then proceeds inward.
Pathophysiology
Pressure ulcers may be caused by inadequate blood supply and resulting reperfusion injury when blood re-enters tissue. A simple example of a mild pressure sore may be experienced by healthy individuals while sitting in the same position for extended periods of time: the dull ache experienced is indicative of impeded blood flow to affected areas. Within 2 hours, this shortage of blood supply, called ischemia, may lead to tissue damage and cell death. The sore will initially start as a red, painful area, which eventually turns purple. Left untreated, the skin may break open and become infected. Moist skin is more sensitive to tissue ischemia and necrosis and is also more likely to get infected.
Epidemiology
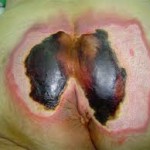 Within acute care in the United States, the incidence of bedsores is 0.4% to 38%; within long-term care, 2.2% to 23.9%; and in home care, 0% to 17%. There is the same wide variation in prevalence: 10% to 18% in acute care, 2.3% to 28% in long-term care, and 0% to 29% in home care. There is a much higher rate of bedsores in intensive care units because of immunocompromised individuals, with 8% to 40% of ICU patients developing bedsores. However pressure ulcer prevalence is highly dependent on the methodology used to collect the data. Using the European Pressure Ulcer Advisory Panel (EPUAP) methodology there is are similar figures for pressure ulcers in acute hospital patients. There are differences across countries, but in Europe (for example) using this methodology pressure ulcer prevalence was consistently high, from 8.3% (Italy) to 22.9% (Sweden). A recent study in Jordan also showed a figure in this range.
Within acute care in the United States, the incidence of bedsores is 0.4% to 38%; within long-term care, 2.2% to 23.9%; and in home care, 0% to 17%. There is the same wide variation in prevalence: 10% to 18% in acute care, 2.3% to 28% in long-term care, and 0% to 29% in home care. There is a much higher rate of bedsores in intensive care units because of immunocompromised individuals, with 8% to 40% of ICU patients developing bedsores. However pressure ulcer prevalence is highly dependent on the methodology used to collect the data. Using the European Pressure Ulcer Advisory Panel (EPUAP) methodology there is are similar figures for pressure ulcers in acute hospital patients. There are differences across countries, but in Europe (for example) using this methodology pressure ulcer prevalence was consistently high, from 8.3% (Italy) to 22.9% (Sweden). A recent study in Jordan also showed a figure in this range.
The risk of developing bedsores can be determined by using the Braden Scale for Predicting Pressure Ulcer Risk.
Treatment
The best treatment outcomes will result from using a multidisciplinary team of specialists, this will ensure all problems are addressed.
There are seven major contributors to healing.
Preventive care
The most important care for a patient with bedsores is the relief of pressure. Once a bedsore is found, pressure should immediately be lifted from the area and the patient turned at least every two hours to avoid aggravating the wound. Nursing homes and hospitals usually set programs to avoid the development of bedsores in bedridden patients such as using a standing frame to reduce pressure and ensuring dry sheets by using catheters or impermeable dressings. For individuals with paralysis, pressure shifting on a regular basis and using a cushion featuring pressure relief components can help prevent pressure wounds.
Pressure-distributive mattresses are used to reduce high values of pressure on prominent or bony areas of the body. Antidecubitus mattresses and cushions can contain multiple air chambers that are alternately pumped. However, methods to evaluate the efficacy of these products have only been developed in recent years.
Debridement
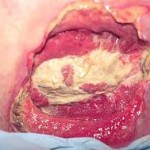 The removal of necrotic tissue is an absolute must in the treatment of pressure sores. Because dead tissue is an ideal area for bacterial growth, it has the ability to greatly compromise wound healing. There are at least seven ways to excise necrotic tissue.
The removal of necrotic tissue is an absolute must in the treatment of pressure sores. Because dead tissue is an ideal area for bacterial growth, it has the ability to greatly compromise wound healing. There are at least seven ways to excise necrotic tissue.
- Autolytic debridement is the use of moist dressings to promote autolysis with the body’s own enzymes. It is a slow process, but mostly painless.
- Biological debridement, or maggot debridement therapy, is the use of medical maggots to feed on necrotic tissue and therefore clean the wound of excess bacteria. Although this fell out of favour for many years, in January 2004, the FDA approved maggots as a live medical device.
- Chemical debridement, or enzymatic debridement, is the use of prescribed enzymes that promote the removal of necrotic tissue.
- Surgical debridement or Sharp Debridement is the most popular  method, as it allows a surgeon to quickly remove dead tissue with little pain to the patient.