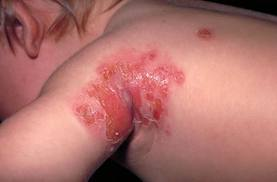
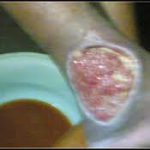
Cellulitis facts
- Cellulitis is a spreading bacterial infection of the skin and tissues beneath the skin.
- Staphylococcus and Streptococcus are the types of bacteria that are usually responsible for cellulitis, although many types of bacteria can cause the condition.
- Sometimes cellulitis appears in areas where the skin has broken open, such as the skin near ulcers or surgical wounds.
- Cellulitis is not contagious.
- Cellulitis is treated with oral or intravenous antibiotics.
What is cellulitis?
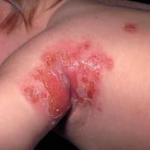 Cellulitis is a bacterial infection of the skin and tissues beneath the skin. Unlike impetigo, which is a very superficial skin infection, cellulitis is an infection that also involves the skin’s deeper layers: the dermis and subcutaneous tissue. The main bacteria responsible for cellulitis are Streptococcus and Staphylococcus (“staph”), the same bacteria that can cause impetigo. MRSA (methicillin-resistant Staph aureus) can also cause cellulitis. Sometimes, other bacteria (for example, Hemophilus influenzae, Pneumococcus, and Clostridium species) may cause cellulitis as well.
Cellulitis is a bacterial infection of the skin and tissues beneath the skin. Unlike impetigo, which is a very superficial skin infection, cellulitis is an infection that also involves the skin’s deeper layers: the dermis and subcutaneous tissue. The main bacteria responsible for cellulitis are Streptococcus and Staphylococcus (“staph”), the same bacteria that can cause impetigo. MRSA (methicillin-resistant Staph aureus) can also cause cellulitis. Sometimes, other bacteria (for example, Hemophilus influenzae, Pneumococcus, and Clostridium species) may cause cellulitis as well.
Cellulitis is fairly common and affects people of all races and ages. Men and women appear to be equally affected. Although cellulitis can occur in people of any age, it is most common in middle-aged and elderly people.
What are cellulitis symptoms and signs?
Cellulitis usually begins as a small area of tenderness, swelling, and redness that spreads to adjacent skin. As this red area begins to enlarge, the affected person may develop a fever, sometimes with chills and sweats, tenderness, and swollen lymph nodes (“swollen glands”) near the area of infected skin.
Where does cellulitis occur?
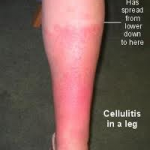
Cellulitis may occur anywhere on the body, but the lower leg is the most common site of the infection (particularly in the area of the tibia or shinbone and in the foot), followed by the arm, and then the head and neck areas. In special circumstances, such as following surgery or trauma wounds, cellulitis can develop in the abdomen or chest areas. People with morbid obesity can also develop cellulitis in the abdominal skin. Special types of cellulitis are sometimes designated by the location of the infection. Examples include periorbital (around the eye socket) cellulitis, buccal (cheek) cellulitis, facial cellulitis, and perianal cellulitis.
What does cellulitis look like?
The signs of cellulitis include redness, warmth, swelling, tenderness, and pain in the involved tissues. Any skin wound or ulcer that exhibits these signs may be developing cellulitis.
Other forms of noninfected inflammation may mimic cellulitis. People with poor leg circulation, for instance, often develop scaly redness on the shins and ankles; this is called “stasis dermatitis” and is often mistaken for the bacterial infection of cellulitis.
What are cellulitis risk factors?
Most commonly, cellulitis develops in the area of a break in the skin, such as a cut, small puncture wound, or insect bite. In some cases when cellulitis develops without an apparent skin injury, it may be due to microscopic cracks in the skin that is inflamed or irritated. It may also appear in the skin near ulcers or surgical wounds.
In other circumstances, cellulitis occurs where there has been no skin break at all, such as with chronic leg swelling (edema). A preexisting skin infection, such as athlete’s foot (tinea pedis) or impetigo can predispose to the development of cellulitis. Likewise, inflammatory conditions of the skin like eczema, psoriasis, or skin damage caused by radiation therapy can lead to cellulitis.
People who have diabetes or conditions that compromise the function of the immune system (for example, HIV/AIDS or those receiving chemotherapy or drugs that suppress the immune system) are particularly prone to developing cellulitis.
 Diabetics are more susceptible to cellulitis than the general population because of impairment of the immune system; they are especially prone to cellulitis in the feet, because the disease causes impairment of blood circulation in the legs, leading to diabetic foot/foot ulcers. Poor control of blood glucose levels allows bacteria to grow more rapidly in the affected tissue, and facilitates rapid progression if the infection enters the bloodstream. Neural degeneration in diabetes means these ulcers may not be painful and thus often become infected.
Diabetics are more susceptible to cellulitis than the general population because of impairment of the immune system; they are especially prone to cellulitis in the feet, because the disease causes impairment of blood circulation in the legs, leading to diabetic foot/foot ulcers. Poor control of blood glucose levels allows bacteria to grow more rapidly in the affected tissue, and facilitates rapid progression if the infection enters the bloodstream. Neural degeneration in diabetes means these ulcers may not be painful and thus often become infected.
Conditions that reduce the circulation of blood in the veins or that reduce circulation of the lymphatic fluid (such as venous insufficiency, obesity, pregnancy, or surgeries) also increase the risk of developing cellulitis.
Cellulitis is also extremely prevalent among dense populations sharing hygiene facilities and common living quarters, such as military installations, college dormitories, nursing homes, oil platforms and homeless shelters. It is advised if a cabin is shared with a sufferer, urgent medical treatment should be given.
What causes cellulitis?
The majority of cellulitis infections are caused by infection with either strep (Streptococcus) or staph (Staphylococcus) bacteria.