Benign prostatic hyperplasia (BPH) is known as one of the most common medical condition in aging men. More than 50% of the male population by the age of 60 is diagnosed with BPH and by the age of 80 years old, the percentage of prevalence is as high as 90%. The development of this condition can start as early as by the age of 40 years old. The disturbing symptoms that BPH bring about cause many problems to patients, which include urination problems, sleeping disturbances, and even daily routines. Nonetheless, this is a treatable disorder. If appropriate management is engaged, complications and mortality are rare with regards to BPH.
 How does BPH develop?
How does BPH develop?
The prostate, being a part of the reproductive organ in the males, is largely affected by the male sex hormone, i.e. androgen hormone, known as dihydrotestosterone (DHT). The action of this hormone ultimately results in increase cellular production, i.e. hyperplasia, causing enlargement of the prostate gland. Unlike women who will undergo menopause and hence cessation of their reproductive function, the prostate continues to respond to the sex hormones, such as testosterone and DHT. Thus, the response of prostate gland to the continuous production of hormones and result in enlargement of the prostate as one grows older.
Anatomically, the prostate gland is located just below the urinary bladder, enveloping part of the urethra. The gland itself is composed of different layers that are categorized in terms of zones or lobes. From the outermost layer they consist of the capsule, then the peripheral, central, anterior, fibromuscular stroma and the transition zones. The transition zone is the one that surrounds the urethra and also the zone that grows throughout life. Thus its continuous enlargement gives rise to BPH.
 What are the signs and symptoms of BPH?
What are the signs and symptoms of BPH?
Due to the enlargement of the transition zone of the prostate, lower urinary tract symptoms (LUTS) contributes to significant symptoms that are bothersome to patients.
- Progressive urinary frequency
- Sense of urgency to urinate
- Difficulty in initiating urination
- The need to strain when urinating
- Poor stream of urinary flow
- Dribbling at the end of urination
- Sense of incomplete voiding
However, not all the patients will have such extend of symptoms which are significant enough to make them want to visit a doctor. The symptoms vary among individuals. It is still best to do a screening test in order to be sure.
Who is at risk of developing BPH?
- Men above 50 years old
- Family history of prostate problems, e.g. father, brother, or uncle
What to expect when I see the doctor?
When you visit a doctor, these will be the list of examination and tests you might have to undergo.
- The America Urological Association Symptom Score for BPH – a set of questionnaire with scoring system is given to patient to fill in to assess the progression of the symptoms. However, please take note that this questionnaire is not for diagnostic purpose. You should consult your physician about your specific medical condition.

Score: 1 -7: Mild      8 – 19: Moderate      20 – 35: Severe
- Digital rectal examination – this is a physical examination where the doctor will insert his/her finger into the rectum to assess the prostate as it lies in front of the rectum.

- Prostate-specific antigen (PSA) levels – High free PSA levels are associated with an enlarged prostate. Although BPH do not cause prostate cancer, it is also advisable to undergo this blood test as a screening for prostate cancer. A level of >4ng/ml permits a prostate biopsy to further evaluate the cytology of the gland.
- Transrectal ultrasonography – a typical ultrasound procedure over the lower abdomen to evaluate the measurement of the prostate.
- Urinalysis – urine dipstick test to rule out urinary tract infection
- Cystoscopy – although this is an invasive procedure, but just like any endoscopy, it is done under sedation and it gives the physician a clear view of what is going on inside the urethra and bladder to rule out other causes of urinary symptoms.
Treatment Options
Medication
- Alpha-adrenergic blockers – these are muscle relaxants that helps improve voiding problems.  Examples include terazosin, doxazosin and tamsulosin.
- 5α-reductase inhibitors – these inhibits the enzyme that metabolise DHT hormones to prevent further enlargement of the prostate gland. Examples include finasteride and dutasteride.
The combination of these two drug therapy significantly improves symptoms compared to using either one of it.
Surgery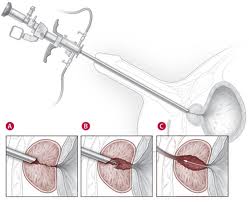
Transurethral resection of the prostate (TURP) – this procedure has been widely accepted as the standard surgical procedure to treat BPH.
Other procedures
There are less invasive procedures which their long-term results of treatment for BPH are still under study. These include, laser ablation, radiofrequency vaporization and high-intensity-focused ultrasound.

Complications of BPH
If medical help is not sought, the following complications can develop.
- Urinary tract infection
- Acute urinary retention

- Hydronephrosis – a condition where the kidney becomes swollen due to accumulation of urine
