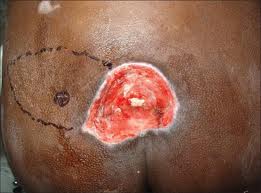
Infection control
Infection has one of the greatest effects on the healing of a wound. Symptoms of systemic infection include fever, pain, redness, swelling, warmth of the area, and purulent discharge. Additionally, infected wounds may have a gangrenous smell, be discoloured, and may eventually exude even more pus.
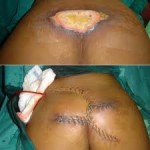 In order to eliminate this problem, it is imperative to apply antiseptics at once. Hydrogen peroxide is not recommended for this task as it is difficult to balance the toxicity of the wound with this. New dressings have been developed that have cadexomer iodine and silver in them, and they are used to treat bad infections. Duoderm can be used on smaller wounds to both provide comfort and protect them from infection.
In order to eliminate this problem, it is imperative to apply antiseptics at once. Hydrogen peroxide is not recommended for this task as it is difficult to balance the toxicity of the wound with this. New dressings have been developed that have cadexomer iodine and silver in them, and they are used to treat bad infections. Duoderm can be used on smaller wounds to both provide comfort and protect them from infection.
Systemic antibiotics are not recommended in treating infection of a bedsore, as it can lead to bacterial resistance.
Nutritional support
Upon admission the patient should have a consultation with a dietitian to determine the best diet to support healing, as a malnourished person does not have the ability to synthesize enough protein to repair tissue. The dietitian should conduct a nutritional assessment that includes a battery of questions and a physical examination. If malnourishment is suspected, lab tests should be run to check serum albumin and lymphocyte counts. Additionally, a bioelectrical impedance analysis should be considered.
If the patient is found to be at risk for malnutrition, it is imperative to begin nutritional intervention with dietary supplements and nutrients including, but not limited to, arginine, glutamine, vitamin A, vitamin B complex, vitamin E, vitamin C, magnesium, manganese, selenium and zinc. It is very important that intake of these vitamins and minerals be overseen by a physician, as many of them can be detrimental in incorrect dosages.
There is anecdotal evidence that high protein diet helps healing of sores. High protein diet seems to be especially helpful in sores that do not heal in eight weeks.
Wound intervention
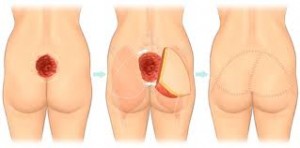 Once the patient has reached the point that intervention is possible, there are many different options. For patients with Stages I and II ulcers, the wound care team should use guidelines established by the American Medical Directors Association (AMDA) for the treatment of these low-grade sores.
Once the patient has reached the point that intervention is possible, there are many different options. For patients with Stages I and II ulcers, the wound care team should use guidelines established by the American Medical Directors Association (AMDA) for the treatment of these low-grade sores.
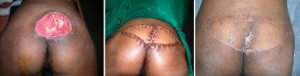
For those with Stage III or IV ulcers, most interventions will likely include surgery such as a tissue flap, free flap or other closure methods. A more recent intervention is Negative Pressure Wound Therapy, which is the application of topical negative pressure to the wound. This technique, developed by scientists at Wake Forest University, uses foam placed into the wound cavity which is then covered in a film which creates an airtight seal. Once this seal is established, the technician is able to remove exudate and other infectious materials in addition to aiding the body produce granulation tissue, the best bed for the creation of new skin.
There are, unfortunately, contraindications to the use of negative pressure therapy. Most deal with the unprepared patient, one who has not gone through the previous steps toward recovery, but there are also wound characteristics that bar a patient from participating: a wound with inadequate circulation, a raw debrided wound, a wound with necrotised tissue and eschar, and a fibrotic wound.
After Negative Pressure Wound Therapy, the patient should be reevaluated every two weeks to determine future therapy.
Prevention
It is common sense that prevention is better than cure – this applies particularly to pressure sores, which are painful and slow to heal, and most of which are definitely preventable if good clinical practice is followed. In the UK the Royal College of Nursing has published guidelines in ‘Pressure ulcer risk assessment and prevention’. It is important to identify those who are at risk and to intervene early with strategies for prevention, in the bed, wheelchair or chair, in the bath and on the commode – indeed, it is a requirement within the National Standards for Care Homes (UK) to do so:
 “Standard 8.3 Service users are assessed, by a person trained to do so, to identify those service users who have developed, or are at risk of developing, pressure sores and appropriate intervention is recorded in the plan of care. 8.4 The incidence of pressure sores, their treatment and outcome, are recorded in the service user’s individual plan of care and reviewed on a continuing basis. 8.5 Equipment necessary for the promotion of tissue viability and prevention or treatment of pressure sores is provided.”
“Standard 8.3 Service users are assessed, by a person trained to do so, to identify those service users who have developed, or are at risk of developing, pressure sores and appropriate intervention is recorded in the plan of care. 8.4 The incidence of pressure sores, their treatment and outcome, are recorded in the service user’s individual plan of care and reviewed on a continuing basis. 8.5 Equipment necessary for the promotion of tissue viability and prevention or treatment of pressure sores is provided.”
A wide variety of techniques are used to mitigate the risk of pressure ulcers in at risk groups including: nutritional supplements, topical skin protection and mechanical devices to mimic the effect of movement, such as alternating pressure mattresses. The most commonly used method of reducing the risk of pressure ulcers is regular nursing intervention and a ‘turning schedule’ to ensure the weight of the immobile patient is redistributed, reducing sustained pressure on a vulnerable area.
Complications
Pressure sores can trigger other ailments, cause patients considerable suffering, and be expensive to treat. Some complications include autonomic dysreflexia, bladder distension, osteomyelitis, pyarthroses, sepsis, amyloidosis, anemia, urethral fistula, gangrene and very rarely malignant transformation (Marjolin’s ulcer – secondary carcinomas in chronic wounds). Sores often recur because patients do not follow recommended treatment or develop seromas, hematomas, infections, or dehiscence. Paralytic patients are the most likely people to have pressure sores recur. In some cases, complications from pressure sores can be life-threatening. The most common causes of fatality stem from renal failure and amyloidosis.