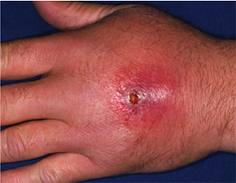
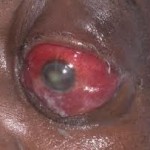
The most common bacteria that cause cellulitis are beta-hemolytic streptococci (groups A, B, C, G, and F). A form of rather superficial cellulitis caused by strep is called erysipelas and is characterized by spreading hot, bright red circumscribed area on the skin with a sharp, raised border. Erysipelas is more common in young children. The so-called “flesh-eating bacteria” are, in fact, also a strain of strep bacteria that can sometimes rapidly destroy tissues underneath the skin.
Staph (Staphylococcus aureus), including methicillin-resistant strains (MRSA), is another common type of bacteria that causes cellulitis. There is a growing incidence of community-acquired infections due to methicillin-resistant S. aureus (MRSA), a particularly dangerous form of this bacteria that is resistant to many antibiotics, including methicillin, and is therefore more difficult to treat.
Cellulitis can be caused by many other types of bacteria. In children under 6 years of age, H. flu (Hemophilus influenzae) bacteria can cause cellulitis, especially on the face, arms, and upper torso. Cellulitis from a dog or cat bite or scratch may be caused by the Pasteurella multocida bacteria, which has a very short incubation period of only four to 24 hours. Aeromonas hydrophilia, Vibrio vulnificus, and other bacteria are causes of cellulitis that develops after exposure to freshwater or seawater. Pseudomonas aeruginosa is another type of bacteria that can cause cellulitis, typically after a puncture wound.
Is cellulitis contagious?
Cellulitis is not contagious because it is an infection of the skin’s deeper layers (the dermis and subcutaneous tissue), and the skin’s top layer (the epidermis) provides a cover over the infection. In this regard, cellulitis is different from impetigo, in which there is a very superficial skin infection that can be contagious.
How is cellulitis diagnosed, and what is the treatment for cellulitis?
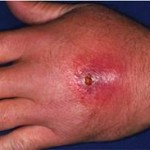 First, it is crucial for the doctor to distinguish whether or not the inflammation is due to an infection. The history and physical exam can provide clues in this regard, as can sometimes an elevated white blood cell count. A culture for bacteria may also be of value, but in many cases of cellulitis, the concentration of bacteria may be low and cultures fail to demonstrate the causative organism. In this situation, cellulitis is commonly treated with antibiotics that are designed to eradicate the most likely bacteria to cause the particular form of cellulitis.
First, it is crucial for the doctor to distinguish whether or not the inflammation is due to an infection. The history and physical exam can provide clues in this regard, as can sometimes an elevated white blood cell count. A culture for bacteria may also be of value, but in many cases of cellulitis, the concentration of bacteria may be low and cultures fail to demonstrate the causative organism. In this situation, cellulitis is commonly treated with antibiotics that are designed to eradicate the most likely bacteria to cause the particular form of cellulitis.
When it is difficult or impossible to distinguish whether or not the inflammation is due to an infection, doctors sometimes treat with antibiotics just to be sure. If the condition does not respond, it may need to be addressed by different methods dealing with types of inflammation that are not infected. For example, if the inflammation is thought to be due to an autoimmune disorder, treatment may be with a corticosteroid.
Antibiotics, such as derivatives of penicillin or other types of antibiotics that are effective against the responsible bacteria, are used to treat cellulitis. If the bacteria turn out to be resistant to the chosen antibiotics, or in patients who are allergic to penicillin, other appropriate antibiotics can be substituted. Sometimes the treatment requires the administration of intravenous antibiotics in a hospital setting, since oral antibiotics may not always provide sufficient penetration of the inflamed tissues to be effective. In certain cases, intravenous antibiotics can be administered at home.
Pain relief is also often prescribed, but excessive pain should always be investigated as it is a symptom of necrotizing fasciitis. Elevation of the affected area is also important. As in other maladies characterized by wounds or tissue destruction, hyperbaric oxygen treatment can be a valuable adjunctive therapy, but is not widely available.
In all cases, physicians choose a treatment based upon many factors, including the location and extent of the infection, the type of bacteria causing the infection, and the overall health status of the patient.
There have been many cases where Lyme disease has been misdiagnosed as staphylococcal- or streptococcal-induced cellulitis. Because the characteristic bullseye rash does not always appear in patients infected with Lyme disease, the similar set of symptoms may be misdiagnosed as cellulitis. Standard treatments for cellulitis are not sufficient for curing Lyme disease. The only way to rule out Lyme disease is with a blood test, which is recommended during warm months in areas where the disease is endemic.
Can cellulitis be prevented?
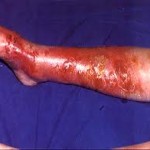 Under some circumstances, cellulitis can be prevented by proper hygiene, treating chronic swelling of tissues (edema), care of wounds or cuts. In other cases, microscopic breaks in the skin may not be apparent and infection may develop. In general, cellulitis in a healthy person with an intact immune system is preventable by avoiding skin surface wounds. In people with predisposing conditions (see above) and/or weakened immune systems, cellulitis may not always be preventable.
Under some circumstances, cellulitis can be prevented by proper hygiene, treating chronic swelling of tissues (edema), care of wounds or cuts. In other cases, microscopic breaks in the skin may not be apparent and infection may develop. In general, cellulitis in a healthy person with an intact immune system is preventable by avoiding skin surface wounds. In people with predisposing conditions (see above) and/or weakened immune systems, cellulitis may not always be preventable.
What is the outlook/prognosis for cellulitis?
Cellulitis is a treatable condition, but antibiotic treatment is necessary to eradicate the infection and avoid spread of the infection. Most cellulitis can be effectively treated with oral antibiotics at home. Sometimes hospitalization and intravenous antibiotics are required if oral antibiotics are not effective. If not properly treated, cellulitis can occasionally spread to the bloodstream and cause a serious bacterial infection of the bloodstream that spreads throughout the body (sepsis).