What is the relationship between cervical cancer and human papilloma virus (HPV)?
It is estimated that up to 80% of women will acquire genital HPV infection at least once in their lifetime regardless of their lifestyles or ages. The risk of HPV infection starts from the first sexual encounter and lasts throughout a woman’s life.
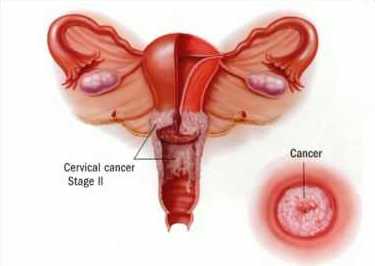 Cervical cancer and HPV have been closely associated together due to evidence from medical research that showed that HPV infection causes pre-malignant lesions in the cervix. If not treated early, these initially benign lesions can undergo cellular changes and ultimately results in cervical cancer.
Cervical cancer and HPV have been closely associated together due to evidence from medical research that showed that HPV infection causes pre-malignant lesions in the cervix. If not treated early, these initially benign lesions can undergo cellular changes and ultimately results in cervical cancer.
What is HPV (human papilloma virus)?
Human papilloma virus (HPV) is a family of more than 100 virus strains that is very common. Of the many different types, some are harmless while others can cause diseases of the genital areas. Most common forms of HPV infections are those types that cause warts. 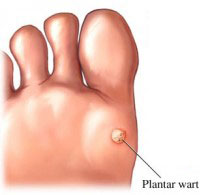 There are also types of HPV that causes oral lesions, such as oral papilloma, laryngeal papillomatosis, or oropharyngeal cancer. However, what concerns the medical community most is the lethal or “high-risk†types of HPV that causes cervical cancer.
There are also types of HPV that causes oral lesions, such as oral papilloma, laryngeal papillomatosis, or oropharyngeal cancer. However, what concerns the medical community most is the lethal or “high-risk†types of HPV that causes cervical cancer.
HPV infection is indeed considered a type of sexually transmitted disease. It is transmitted through genital skin-to-skin contact, so it can affect virtually any woman irrespective of her age or lifestyle. Transmission can occur even without penetrative sex. It is estimated that four out of five sexually active women will have an HPV infection during their lifetime, even if they’ve only had one or two sexual partners. Hence, it does not matter if you are married or not, every woman is at risk of HPV infection throughout her life.
- Sexual intercourse is not necessary to become infected by HPV
- Condoms reduce the risk, but are not fully protective from HPV transmission
- HPV infections can occur without any symptoms
- Majority of HPV infections will be cleared naturally by the body without medical treatment over the course of a few months
- Persistent infection with HPV is what causes the risk of progression to cervical cancer. This process can take more than ten years
What is the Relationship between HPV and Cervical Cancer?
As mentioned above, there are types of HPV that falls under the high-risk category of causing genital diseases, which includes cervical cancer and even anal cancer. These high-risk HPV types are types 16 and 18. They are found in up to 90% of invasive cervical cancer.
Both high-risk and low-risk types of HPV cause abnormal changes to the cervical cells. Nonetheless, research has shown that only the high-risk HPV types lead to cancer. Sometimes, HPV infections can persist for many years. Persistent infections with high-risk HPVs are the primary cause of cervical cancer.
What are the Risk Factors for HPV and Cervical Cancer?
Number of Sexual Partners
As with any sexually transmitted diseases, the more sexual partners you have, the greater the chance of contracting a genital HPV infection. But this does not apply to only you, if your sexual partner have or have had multiple sexual partners before, the risk of you being infected is increased as well.
Multiple Childbirth
Multiparity or multiple childbirth is suggested to be associated with high risk of developing cervical cancer. This could be due to the hormonal and structural changes in the uterus and cervix that a mother undergoes during pregnancy, and also the mechanical trauma to the cervix during the process of giving birth.
 Smoking
Smoking
Being one of the popular risk factor as in other diseases, smoking is one of the most important risk factors in developing cervical cancer. Research has shown that cigarette smoking can cause gene alterations that can lead to abnormal cellular changes of cervical cancer. It is evident that smoking increases the risk of cervical cancer among female who are infected with HPV.
Weak Immune System
Generally, immunocompromised people, as the term suggests, has greater risk of infection. These include patients with autoimmune diseases who are taking immunosuppressive drugs, and also HIV or AIDS patients.
Unprotected Sex

Usage of condom does not fully protect one from contracting HPV infection or any sexually transmitted disease as a matter of fact.However, better be safe than sorry. Condom does reduce the risk of HPV infection to a certain extent.
It is important to know that in any kind of disease, it is a multi-factorial cause that leads to its development. There is no single cause that contributes to cancer. Combinations of risk factors and causes such as persistent HPV infection, multiple childbirth and smoking remain as the main components of the development of cervical cancer. Breakthrough measures have been provided to the public to help early detection of cervical cellular changes and to prevent cervical cancer, such as the Pap smear screening and the HPV vaccines. The decision to protect yourself is up to you.

