What is radiation therapy?
Radiation therapy is a form of cancer treatment that uses high levels of radiation to kill cancer cells or keep them from growing and dividing — while minimizing damage to healthy cells. When used for breast cancer treatment, radiation is delivered to the affected breast and, in some cases, to the lymph nodes under the arm or at the collarbone.
What is MammoSite 5-Day Targeted Radiation Therapy?
 The MammoSite® Radiation Therapy System received FDA clearance in 2002. Since then, over 50,000 women have been treated.
The MammoSite® Radiation Therapy System received FDA clearance in 2002. Since then, over 50,000 women have been treated.
MammoSite Targeted Radiation Therapy works from the inside, meaning that a higher daily dose can be used for a shorter period of time – 5 days vs. 5-7 weeks.
Advantages of MammoSite
- Treatment with MammoSite 5-Day Targeted Radiation Therapy can help you get back to your normal life sooner – just 5 days vs. 5-7 weeks.
- MammoSite places the radiation source inside the lumpectomy cavity (the space left when a tumor is removed). This delivers radiation to the area where cancer is most likely to recur.
- Clinical trials for the MammoSite Radiation Therapy System have shown it to be well tolerated, with mild side effects for a short period of time.
- The therapy is given on an outpatient basis. No hospital stay is required.
- 5-year Initial Clinical Trial Results (N=43):
- No local recurrences
- 83.3% of the patients had good/excellent cosmetic results
- 100% of patients in the initial clinical trial would recommend MammoSite to a friend or family member.
- 100% of patients in the initial clinical trial would use MammoSite again if they had to do it over.
MammoSite vs. External Beam Radiation
Dr. Louis Munoz, radiation oncologist, describes the difference between conventional radiation and MammoSite 5-Day treatment
How It Works
1. Placement
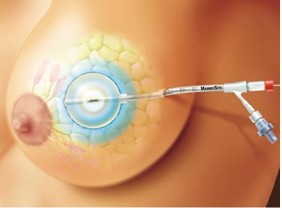
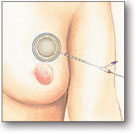
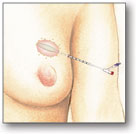 After the breast cancer tumor is removed (lumpectomy), a small, soft MammoSite balloon attached to a thin tube (catheter) is placed inside the lumpectomy cavity through a small incision in the breast.
After the breast cancer tumor is removed (lumpectomy), a small, soft MammoSite balloon attached to a thin tube (catheter) is placed inside the lumpectomy cavity through a small incision in the breast.
- The balloon is “inflated†with saline solution so that it fits snugly into the cavity. It remains inflated during the 5-day treatment.
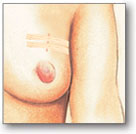
- A small portion of the catheter remains outside the breast; this is secured to a cushioned gauze pad to prevent movement of the catheter.
2. Treatment
- Treatment is planned by a radiation oncologist who will take images of the MammoSite balloon catheter in the breast and determine the amount of radiation needed.
- During therapy, the portion of the catheter that remains outside your breast is connected to a computer-controlled High Dose Rate (HDR) machine that inserts a radiation “seed†to deliver the therapy.
- Once therapy is complete, the seed is removed, the catheter is unplugged, and you will be free to return to your normal daily activities.
- No radiation remains inside your breast in between treatments.
3. Removal
- After 5 days of treatment, your MammoSite balloon catheter will be removed, usually on the last day of treatment.
- The balloon is gently removed through the same incision made to place it.
What to Expect
Clinical studies of the MammoSite® Radiation Therapy System have shown it to be well tolerated, with mild side effects that generally last for a short period of time.5
Side effects that occurred most frequently include redness, bruising and breast pain. These did not occur in all patients.
These are all common side effects of breast surgery and/or radiation therapy and usually go away after a short time.
Occasionally, there is also drainage that occurs from the catheter insertion site, which is normal; this should also go away after a short time.
Even qualified candidates may not complete the 5-day treatment due to varying clinical conditions. In that event, you need to consult your physician about alternate treatments. You should talk to your doctor about all the risks and benefits of your treatment.
Am I a candidate for MammoSite 5-Day Targeted Radiation Therapy?
Four medical societies have created guidelines to help doctors select patients who can benefit from MammoSite 5-Day Targeted Radiation Therapy.
| Professional Medical Society Consensus Guidelines: Patient Selection Criteria for Accelerated Partial Breast Irradiation |
|||||
| ABS1 | ASBS2 | ACRO3 | ASTRO4 | ||
| Suitable | Cautionary | ||||
| Age | ≥50 | ≥45 | ≥45 | ≥60 | 50-59 |
| Diagnosis | Unifocal, invasive ductal carcinoma | Invasive ductal carcinoma or ductal carcinoma in situ (DCIS) | Invasive ductal carcinoma or DCIS | Invasive ductal or other favorable subtypes (ie: mucinous, tubular, colloid) | Pure DCIS ≤3cm EIC ≤3cm |
| Tumor Size | ≤3cm | ≤3cm | ≤3cm | ≤2cm | 2.1-3.0cm |
| Surgical Margins | Negative microscopic margins of excision | Negative microscopic surgical margins of excision | Negative microscopic surgical margins of excision | Negative by at least 2mm | Close (<2mm) |
| Nodal Status | NØ | NØ | NØ | NØ (i-,i+) | |
1M.Keisch, et al. Breast Brachytherapy Task Group, American Brachytherapy Society. February, 2007. http://www.Americanbrachytherapy.org
2Consensus statement for accelerated partial breast irradiation. The American Society of Breast Surgeons. December 8, 2005.
3American College of Radiation Oncology Statement on Partial Breast Irradiation. September, 2008.
4American Society for Radiation Oncology Consensus Statement on Partial Breast Irradiation. July 2009