An acquired brain injury (ABI) is the impairment of normal brain function due to a neurological insult, such as: open or closed head injuries (traumatic brain injury or T.B.I.), select cerebral vascular lesions (i.e., aneurysm, hemorrhage, brain stem stroke), hypoxic event, intracranial tumor, select neurological diseases (i.e., encephalopathy). Well, that is a technical definition. Not very
satisfying, is it? It’s very impersonal and doesn’t really even begin to answer the question. For something as complex as brain injury, there are no easy definitions or answers.
***Most often, brain damage from congenital or genetic origins or birth trauma is not included within the standard definition of A.B.I. Neither are degenerative neurological diseases or disabilities stemming from mental illness. However, the definition of A.B.I. will vary from organization to organization.
HOW DO WE RECOGNIZE AN ACQUIRED BRAIN INJURY?
Acquired Brain Injury has many levels of intensity. It is possible that someone can acquire a brain injury without loss of consciousness or external bruising or tangible confirmation (i.e., CAT Scans, Skull X-rays, EEGs, etc.). Individuals who have
even a mild brain injury may continue to experience a wide variety of symptoms than can have life-changing implications. Keep in mind, however, that brain injury is different and unique for each person.
WHAT ARE THE SIGNS/SYMPTOMS & EFFECTS OF AN ABI?
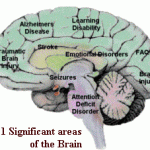
Symptoms and related effects fall into four major groups: Cognitive, Perceptual, Physical and Behavioral/Emotional. Keep in mind that because of the uniqueness of each injury, some survivors may or may not face or exhibit some or all of the symptoms. The number of symptoms does not reflect on the impact that the injury will have on the survivors. Much of that depends on where the injury is located. The following is, by no means, a complete or comprehensive listing.
Cognitive
- Difficulty in processing information – decreased speed, accuracy and consistency
- Shortened attention span
- Inability to understand abstract concepts
- Impaired decision-making ability
- Inability to shift mental tasks or to follow multi-step directions
- Memory loss or impairment
- Language deficits – difficulty expressing thoughts and understanding others, inappropriate word selection
Perceptual
- Change in vision, hearing or sense of touch
- Loss of sense of time and space and spatial disorientation
- Disorders of smell and taste
- Altered sense of balance
- Increased pain sensitivity
Physical
- Persistent headache
- Extreme mental and/or physical fatigue
- Disorders of movement – gaiting, ataxia, spasticity and tremors
- Seizure activity (traumatic epilepsy)
- Impaired small motor control
- Photosensitivity (sensitivity to light)
- Sleep disorders
- Paralysis
- Speech that is not clear due to poor control of the muscles in the lips, tongue and jaw and/or poor breathing patterns.
Behavioral and Emotional
- Irritability and Impatience
- Reduced tolerance for stress
- Lack of initiative – apathy
- Dependence – failure to assume responsibility for one’s actions
- Denial of disability
- Lack of inhibition – may result in aggression, cursing and inappropriate sexual behavior
- Inflexibility
- Flattened or Heightened emotional responses/reactions
How the patient copes with the injury has been found to influence the level at which they experience the emotionally complications correlated with ABI. Three coping strategies for emotions related to ABI have presented themselves in the research, approach-oriented coping, passive coping and avoidant coping.
Approach-oriented coping has been found to be the most effective strategy, it has been negatively correlated with rates of apathy and depression in ABI patients, this coping style is present in individuals who consciously work to minimize the emotional challenges of ABI.
Passive coping has been characterized by the person choosing not to express emotions and a lack of motivation which can lead to poor outcomes for the individual. Increased levels of depression have been correlated to avoidance coping methods in patients with ABI, this strategy is represented in people who actively evade coping with emotions.
These challenges and coping strategies should be kept in consideration when seeking to understand individuals suffering from ABI.
EFFECT ON CHILDREN AND YOUTH
In children and youth with ABI the cognitive and emotional difficulties that stem from their injury can negatively impact their level of participation in home, school and other social situations, participation in structured events has been found to be especially hindered under these circumstances. Involvement in social situations is important for the normal development of children as a means of gaining an understanding of how to effectively work together with others. Furthermore, young people with ABI are often reported as having insufficient problem solving skills. This has the potential to hinder their performance in various academic and social settings further. It is important for rehabilitation programs to deal with these challenges specific to children who have not fully developed at the time of their injury.
HOW LONG WILL IT TAKE TO RECOVER FROM AN ACQUIRED BRAIN INJURY?
Each injury is different and unique to the survivor and all survivors have different capacities for recognizing and compensating for the symptoms they exhibit. Much depends on getting the correct diagnosis and treatment and ensuring that good support
systems are in place for the entire family. Changes and improvements continue although sometimes they are so slight they are hard to notice. It doesn’t happen overnight!