Having an issue with axillary hyperhidrosis can be difficult to deal with given the stigma that society has perpetuated about sweaty people. The fact of the matter is that we all sweat at some level. Now the ones that sweat immensely are in a different boat, but at the same time they can use common methods to help slow down the release of perspiration.
Classification
 Hyperhidrosis can either be generalized or localized to specific parts of the body. Hands, feet, armpits, and the groin area are among the most active regions of perspiration due to the relatively high concentration of sweat glands; however, any part of the body may be affected.
Hyperhidrosis can either be generalized or localized to specific parts of the body. Hands, feet, armpits, and the groin area are among the most active regions of perspiration due to the relatively high concentration of sweat glands; however, any part of the body may be affected.
Hyperhidrosis can also be classified depending by onset, congenital or acquired. Primary hyperhidrosis is found to start during adolescence or even before and seems to be inherited as an autosomal dominant genetic trait. Primary hyperhidrosis must be distinguished from secondary hyperhidrosis, which can start at any point in life. The latter form may be due to a disorder of the thyroid or pituitary gland, diabetes mellitus, tumors, gout, menopause, certain drugs, or mercury poisoning.
Hyperhidrosis may be also divided into palmoplantar (symptomatic sweating of primarily the hands or feet), gustatory and generalized hyperhidrosis.
Alternatively, hyperhidrosis may be classified according to the amount of skin that is affected and its possible causes. In this approach, excessive sweating in an area that is greater than 100 cm2 (up to generalized sweating of the entire body) is differentiated from sweating that affects only a small area.
Cause
The cause of primary hyperhidrosis is unknown, although some surgeons claim that it is caused by sympathetic overactivity. Nervousness or excitement can exacerbate the situation for many sufferers. Other factors can play a role; certain foods and drinks, nicotine, caffeine, and smells can trigger a response.
A common complaint of patients is that they get nervous because they sweat, then sweat more because they are nervous.
Hyperhidrosis of a relatively large area (>100 square cm or generalized)
- In people with a past history of spinal cord injuries
- Autonomic dysreflexia
- Orthostatic hypotension
- Posttraumatic syringomyelia
- Associated with peripheral neuropathies
- Familial dysautonomia (Riley-Day syndrome)
- Congenital autonomic dysfunction with universal pain loss
- Exposure to cold, notably associated with cold-induced sweating syndrome
- Associated with probable brain lesions
- Episodic with hypothermia (Hines and Bannick syndrome)
- Episodic without hypothermia
- Olfactory
- Associated with intrathoracic neoplasms or lesions
- Associated with systemic medical problems
- Pheochromocytoma
- Parkinson’s disease
- Thyrotoxicosis
- Diabetes mellitus
- Congestive heart failure
- Anxiety
- Menopausal state
- Due to drugs or poisoning
- Night sweats
- Compensatory
- Associated with toxins
- Infantile acrodynia induced by chronic low-dose mercury exposure, leading to elevated catecholamine accumulation and resulting in a clinical picture resembling pheochromocytoma.
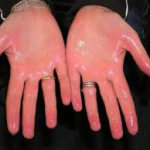 Hyperhidrosis of relatively small area (<100 square cm)
Hyperhidrosis of relatively small area (<100 square cm)
- Idiopathic unilateral circumscribed hyperhydrosis
- Reported association with:
- Blue rubber bleb nevus
- Glomus tumor
- POEMS syndrome
- Burning feet syndrome (Goplan’s)
- Trench foot
- Causalgia
- Pachydermoperiostosis
- Pretibial myxedema
- Gustatory sweating associated with:
- Encephalitis
- Syringomyelia
- Diabetic neuropathies
- Herpes zoster (shingles)
- Parotitis
- Parotid abscesses
- Thoracic sympathectomy
- Auriculotemporal or Frey’s syndrome
- Miscellaneous
- Lacrimal sweating (due to postganglionic sympathetic deficit, often seen in Raeder’s syndrome)
- Harlequin syndrome
- Emotional hyperhydrosis
Treatment
There is a variety of hyperhidrosis treatment available including prevention methods, psychology reconditioning and surgery. One of the cheapest and easiest forms of axillary hyperhidrosis treatment is using deodorants and underarm sweat pads. The combination can help reduce the condition significantly. Sometimes this is not enough, and the next step is to discovery your mental state. First off, the obvious choice to reduce sweating would be an anti-perspiring. The word anti means to oppose, essentially it is a mixture of ingredients that attempts to stop sweat from forming.
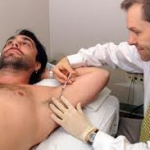 The more severe forms of hyperhidrosis need to be addresses with stronger sweat blockers. The main thing to remember is that sweating begins from your sympathetic nervous system. If the nerves that control sweating are not functioning at optimal levels there could be a chance that this condition becomes aggravated.
The more severe forms of hyperhidrosis need to be addresses with stronger sweat blockers. The main thing to remember is that sweating begins from your sympathetic nervous system. If the nerves that control sweating are not functioning at optimal levels there could be a chance that this condition becomes aggravated.
There is also other prescription based medications that can help prevent underarm sweating such as Aluminum Chloride. Though is this also the main ingredient placed in regular over the counter anti-perspiring bars, stronger forms are available. This axillary hyperhidrosis treatment option should be utilized under supervision because excessive amounts of aluminum are not beneficial to long term health.
It is common for individuals who suffer from anxiety issues to have an excessive sweating problem. Usually, as the stresses everyday life takes their toll on the human mind; individuals tend to sweat more often. For example, if you have to do a presentation in front of your coworkers, this can trigger excessive sweating because of the nervousness that can be associated with public speaking. Attempting to take control of your anxiety and nervousness along with regular prevention methods can help eliminate hyperhidrosis.
If the two options above do not help combat the problem, the final option is axillary hyperhidrosis surgery. The procedure Endoscopic Thoracic Sympathetcomy also known as ETS is done by a thoracic surgeon. The surgery stops the signal transmissions of the sympathetic nerve impulse to the sweat glands, essentially stopping your body from producing sweat in certain regions of the body such as armpits, palms and feet.
Another treatment option is botox axillary hyperhidrosis, which is a temporary method to stop excessive sweating through an injection. There is also oral medication available such as Drysol and Drionic.
Overall, each individuals form of axillary hyperhidrosis treatment will vary based on their needs. For some, it might be as simple as using sweat pads and a strong deodorant while others may need surgical treatment procedures to rid themselves of this potentially life altering condition. The best advice is to pay close attention to what alternatives are working for you and reduce unnecessary stress and anxiety out of your life to combat the condition of axillary hyperhydrosis.
