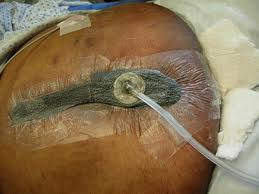
NPWT or negative pressure wound therapy  is already a common modality in proper wound care. It is a method used to treat chronic and acute wounds and in graft fixation. Negative pressure wound therapy is known to help accelerate the process of wound healing by filling the wound with rough granulated tissue and by sealing the wound by closing its edges.
Although it is a very effective treatment, negative pressure wound therapy is not to be used on wounds with cancer cells, osteomyelitis around the wound that is untreated, wounds with a fistula around it, and wounds with necrotic tissue. It is important for your wound to be well-assessed before negative pressure wound therapy is used on it. Here are more facts about negative pressure wound therapy that you can discuss with your doctor:
1. Wound staging
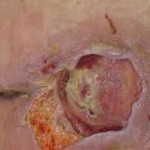 Before negative pressure wound therapy is used, wound staging should be made. Stage one has an erythema that is non-blanchable on light skin and violet or dark on skin with dark pigmention. Stage two is a wound that is partially thick and there is skin loss that affects the dermis or epidermis. Stage three is a wound that has reached full thickness; the skin loss has necrosis or damage to the subcutaneous tissue that is possible to go deep into the fascia. Stage four is a wound that has also reached full thickness with heavily damaged or severely necrotized supporting structures, bone, or muscles.
Before negative pressure wound therapy is used, wound staging should be made. Stage one has an erythema that is non-blanchable on light skin and violet or dark on skin with dark pigmention. Stage two is a wound that is partially thick and there is skin loss that affects the dermis or epidermis. Stage three is a wound that has reached full thickness; the skin loss has necrosis or damage to the subcutaneous tissue that is possible to go deep into the fascia. Stage four is a wound that has also reached full thickness with heavily damaged or severely necrotized supporting structures, bone, or muscles.
2. Procedure
 Negative pressure wound therapy is done systematically with the following steps:
Negative pressure wound therapy is done systematically with the following steps:
- A suction pump is used for varied settings for various types of wounds or patients. Pressure ranging from 70 mmHg to 200 mmHg can be used.
- This suction action will be left for hours during the day, everyday as prescribed.
- The pump is connected to the wound and wound dressings.
- When everything is set up, the pump is switched on. There is contraction of the dressing because of the vacuum effect.
- There is usually discomfort when the pump is first turned on but there are methods to alleviate this.
3. Home setting
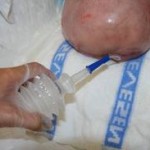 Before negative pressure wound therapy is performed, the dressings should maintain a moist environment for the wound; the necrotic tissue will undergo debridement; the wound will be measured and evaluated by a medical professional; and proper nutrition is provided. For ulcers at stages three or four, the patient will be properly positioned; proper support will be given (group two or three support surface); and the patient’s incontinence and moisture status are managed. For neuropathic or diabetic ulcers, the patient has undergone a program that manages diabetes and proper modalities have been used to reduce the foot pressure. For ulcers with insufficient venous circulation, compression garments or bandages are applied and ambulation or elevation of the affected leg is facilitated and encouraged.
Before negative pressure wound therapy is performed, the dressings should maintain a moist environment for the wound; the necrotic tissue will undergo debridement; the wound will be measured and evaluated by a medical professional; and proper nutrition is provided. For ulcers at stages three or four, the patient will be properly positioned; proper support will be given (group two or three support surface); and the patient’s incontinence and moisture status are managed. For neuropathic or diabetic ulcers, the patient has undergone a program that manages diabetes and proper modalities have been used to reduce the foot pressure. For ulcers with insufficient venous circulation, compression garments or bandages are applied and ambulation or elevation of the affected leg is facilitated and encouraged.
4. In-patient setting
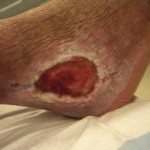 If the wounds mentioned earlier were in in-patient setting, negative pressure wound therapy will be performed. If the patient has experienced dehiscence after surgery or of the wound was traumatic, negative pressure wound therapy will also be done. Note that pumps for negative pressure wound therapy must be able to accommodate more than a single set for wound dressing for several woundS on the patient.
If the wounds mentioned earlier were in in-patient setting, negative pressure wound therapy will be performed. If the patient has experienced dehiscence after surgery or of the wound was traumatic, negative pressure wound therapy will also be done. Note that pumps for negative pressure wound therapy must be able to accommodate more than a single set for wound dressing for several woundS on the patient.
5. CMN (Continued Medical Necessity)
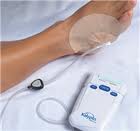 If negative pressure wound therapy should be done continuously, the healthcare professional will conduct the method on a regular basis and directly supervise the negative pressure wound therapy changes in dressings. The wound will be monitored and assessed monthly. The appearance and condition will be properly documented.
If negative pressure wound therapy should be done continuously, the healthcare professional will conduct the method on a regular basis and directly supervise the negative pressure wound therapy changes in dressings. The wound will be monitored and assessed monthly. The appearance and condition will be properly documented.
6. Discontinuation
 The negative pressure wound therapy will be discontinued when the wound has already healed to a certain favorable degree; if four months have already been spent on negative pressure wound therapy; and if the supplies or equipment are no longer used for the patient (doctor’s order or not).
The negative pressure wound therapy will be discontinued when the wound has already healed to a certain favorable degree; if four months have already been spent on negative pressure wound therapy; and if the supplies or equipment are no longer used for the patient (doctor’s order or not).
7. Supplies used
 For the application of negative pressure wound therapy, fifteen wound dressing kits should be used on the patient for an entire month, unless it is necessary for the patient to have one wound dressing kit per change. A limit of up to 10 sets of canisters should be used per month unless there is more than 90 milliliters of wound discharge everyday. If there is a very large amount of wound exudates, a fixed pump with a large canister should be utilized.
For the application of negative pressure wound therapy, fifteen wound dressing kits should be used on the patient for an entire month, unless it is necessary for the patient to have one wound dressing kit per change. A limit of up to 10 sets of canisters should be used per month unless there is more than 90 milliliters of wound discharge everyday. If there is a very large amount of wound exudates, a fixed pump with a large canister should be utilized.
The negative pressure wound therapy will only work with proper administration by a licensed healthcare professional, using the aseptic method. You should discuss this procedure very well with your doctor so as to know the risks and proper follow-up procedures to consider.