To ensure that Medicare pays for your shoes, you must follow the steps below:
Your treating doctor must complete a certificate of medical necessity for the therapeutic shoes and document the need in your medical records. Do not order anything until you have visited your doctor – no matter what the sales person tells you.
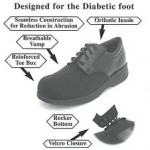 Â Â Â Â Â The shoes and inserts must be prescribed by a podiatrist or other qualified doctor and provided by a podiatrist, orthotist, prosthetist, or pedorthist.
     The shoes and inserts must be prescribed by a podiatrist or other qualified doctor and provided by a podiatrist, orthotist, prosthetist, or pedorthist.
The supplier must receive the order before Medicare is billed and must keep it on file.
If you receive your Medicare through a Medicare Advantage Plan (like an HMO or PPO) it is likely you will have to follow the plan’s steps for approval and purchase. Make a point of calling your plan’s customer service number and ask about their steps for coverage of diabetic shoes.
Medicare will cover one of the following per calendar year:
One pair of depth-inlay shoes and three pairs of inserts or;
One pair of custom molded shoes (including inserts) and two additional pairs of inserts. This option is only available if you cannot wear depth-inlay shoes due to a foot deformity.
In certain cases, Medicare may also cover separate inserts or shoe modifications instead of inserts.
Medicare will not cover deluxe features: A deluxe feature is one that does not contribute to the shoe’s therapeutic function – for example, a custom style, color or custom material.
How Do I Qualify for the Coverage of Diabetic Shoes?
You must be covered under Medicare Part B and all three of the following conditions are met:
1. You have diabetes and;
2. You have one or more of the following conditions:
Partial or complete foot amputation
Past foot ulcers
Calluses of either foot that could lead to ulcers
Nerve damage in your feet with signs of calluses on either foot
Deformity of either foot (for example, hammertoe or bunions)
Poor circulation in either foot.
3. Your doctor has certified your need in writing, and it states that:
 Â Â Â Â Â You meet the criteria for the shoes
     You meet the criteria for the shoes
The doctor (must be an M.D. or D.O.) is treating you under a comprehensive plan of care for diabetes
The exact reasons you need the therapeutic shoes and/or inserts
Remember:
Only an M.D. or D.O. can sign the certification statement; a podiatrist may write the prescription for the shoes, but the M.D. or D.O. who is treating your diabetic condition must certify it. While a podiatrist can prescribe diabetic shoes, they cannot sign the physician’s certification statement.
You will need a new order for the replacement of any shoe
A copy of the certification statement and prescription must be kept on file by your supplier
A new certification statement will be required for shoes, inserts or modifications each year they are purchased
How Much Will Diabetic Shoes Cost Me?
How much you pay will depend on whether or not you have Part B coverage and where you buy your shoes. However, if you are enrolled in Medicare Part B these general rules apply:
After you have paid your yearly deductible, you will pay 20% of the approved Medicare amount for the shoes and inserts.
You will pay less if you buy from a supplier who accepts assignment. If you receive your Medicare through a Medicare Advantage Health Plan, you may owe little to nothing depending on the plan with which you have signed up and your benefits with the plan. If you have a Medigap/Medicare Supplemental plan, you might owe little to no money for your shoes.
It is important to do your homework. Read about the factors that affect how much coverage you will receive. Make sure all paperwork is completed correctly and that you buy through an approved supplier that accepts assignment.
Where Do I Buy Diabetic Shoes?
 You will save money if you order from a Medicare-approved provider. If the supplier from which you order your shoes is not enrolled in Medicare, Medicare will not pay for the shoes.
You will save money if you order from a Medicare-approved provider. If the supplier from which you order your shoes is not enrolled in Medicare, Medicare will not pay for the shoes.
Things you should think about before you choose a supplier:
There are two types of Medicare suppliers: participating suppliers, and those who are enrolled but have chosen not to participate.
Participating suppliers must accept assignment.
A Medicare-approved provider who does not want to participate can charge more than the Medicare-approved amount. However, they cannot charge more than 15% above the Medicare-approved amount. They may also ask you to pay the entire bill when you pick up the shoes. In this situation, Medicare will send the reimbursement directly to you. However, be prepared to wait; it may take a couple of months to receive payment.
If you receive your Medicare coverage through a Medicare Advantage Plan (like an HMO or PPO), it is likely that the plan will have its own steps for shoe purchases. In addition, the plan may have restrictions on the supplier from which you can buy. It is important to know that your health plan must supply at least what Medicare covers — they cannot supply less. Depending on your plan, you may actually receive more coverage than you would get with Medicare alone. It is wise to call your Medicare Advantage Plan’s customer service and ask about your coverage before you order diabetic shoes.
