Arm–leg gradient
The arm–leg (blood pressure) gradient is the difference between the blood pressure measured in the arms and that measured in the legs. It is normally less than 10 mmHg, but may be increased in e.g. coarctation of the aorta.
Vascular resistance
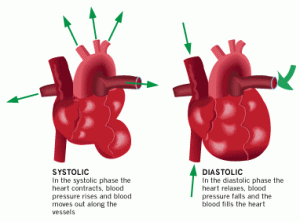 The larger arteries, including all large enough to see without magnification, are conduits with low vascular resistance (assuming no advanced atherosclerotic changes) with high flow rates that generate only small drops in pressure. The smaller arteries and arterioles have higher resistance, and confer the main drop in blood pressure along the circulatory system.
The larger arteries, including all large enough to see without magnification, are conduits with low vascular resistance (assuming no advanced atherosclerotic changes) with high flow rates that generate only small drops in pressure. The smaller arteries and arterioles have higher resistance, and confer the main drop in blood pressure along the circulatory system.
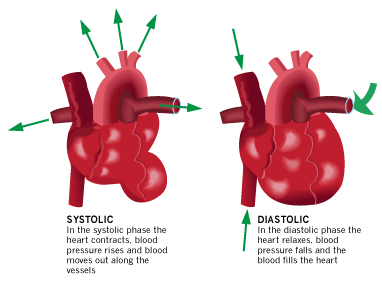
Vascular pressure wave
Modern physiology developed the concept of the vascular pressure wave (VPW). This wave is created by the heart during the systole and originates in the ascending aorta. Much faster than the stream of blood itself, it is then transported through the vessel walls to the peripheral arteries. There the pressure wave can be palpated as the peripheral pulse. As the wave is reflected at the peripheral veins, it runs back in a centripetal fashion. When the reflected wave meets the next outbound pressure wave, the pressure inside the vessel rises higher than the pressure in the aorta. This concept explains why the arterial pressure inside the peripheral arteries of the legs and arms is higher than the arterial pressure in the aorta, and in turn for the higher pressures seen at the ankle compared to the arm with normal ankle brachial pressure index values.
Regulation
 The endogenous regulation of arterial pressure is not completely understood, but the following mechanisms of regulating arterial pressure have been well-characterized:
The endogenous regulation of arterial pressure is not completely understood, but the following mechanisms of regulating arterial pressure have been well-characterized:
- Baroreceptor reflex: Baroreceptors in the high pressure receptor zones (mainly in the aortic arch and carotid sinus) detect changes in arterial pressure. These baroreceptors send signals ultimately to the medulla of the brain stem, specifically to the Rostral ventrolateral medulla (RVLM). The medulla, by way of the autonomic nervous system, adjusts the mean arterial pressure by altering both the force and speed of the heart’s contractions, as well as the total peripheral resistance. The most important arterial baroreceptors are located in the left and right carotid sinuses and in the aortic arch.
- Renin-angiotensin system (RAS): This system is generally known for its long-term adjustment of arterial pressure. This system allows the kidney to compensate for loss in blood volume or drops in arterial pressure by activating an endogenous vasoconstrictor known as angiotensin II.
- Aldosterone release: This steroid hormone is released from the adrenal cortex in response to angiotensin II or high serum potassium levels. Aldosterone stimulates sodium retention and potassium excretion by the kidneys. Since sodium is the main     ion that determines the amount of fluid in the blood vessels by osmosis, aldosterone will increase fluid retention, and indirectly, arterial pressure.
- Baroreceptors in low pressure receptor zones (mainly in the venae cavae and the pulmonary veins, and in the atria) result in feedback by regulating the secretion of antidiuretic hormone (ADH/Vasopressin), renin and aldosterone. The resultant increase in blood volume results an increased cardiac output by the Frank–Starling law of the heart, in turn increasing arterial blood pressure.
These different mechanisms are not necessarily independent of each other, as indicated by the link between the RAS and aldosterone release. Currently, the RAS is targeted pharmacologically by ACE inhibitors and angiotensin II receptor antagonists. The aldosterone system is directly targeted by spironolactone, an aldosterone antagonist. The fluid retention may be targeted by diuretics; the antihypertensive effect of diuretics is due to its effect on blood volume. Generally, the baroreceptor reflex is not targeted in hypertension because if blocked, individuals may suffer from orthostatic hypotension and fainting.
Normal
 While average values for arterial pressure could be computed for any given population, there is often a large variation from person to person; arterial pressure also varies in individuals from moment to moment. Additionally, the average of any given population may have a questionable correlation with its general health; thus the relevance of such average values is equally questionable. However, in a study of 100 human subjects with no known history of hypertension, an average blood pressure of 112/64 mmHg was found, which are currently classified as desirable or “normal” values. Normal values fluctuate through the 24-hour cycle, with highest readings in the afternoons and lowest readings at night.
While average values for arterial pressure could be computed for any given population, there is often a large variation from person to person; arterial pressure also varies in individuals from moment to moment. Additionally, the average of any given population may have a questionable correlation with its general health; thus the relevance of such average values is equally questionable. However, in a study of 100 human subjects with no known history of hypertension, an average blood pressure of 112/64 mmHg was found, which are currently classified as desirable or “normal” values. Normal values fluctuate through the 24-hour cycle, with highest readings in the afternoons and lowest readings at night.
Clinical trials demonstrate that people who maintain arterial pressures at the low end of these pressure ranges have much better long term cardiovascular health. The principal medical debate concerns the aggressiveness and relative value of methods used to lower pressures into this range for those who do not maintain such pressure on their own. Elevations, more commonly seen in older people, though often considered normal, are associated with increased morbidity and mortality.
Average blood pressure in (mmHg):
|
1 year |
6–9 years |
adults  |
| 95/65 | 100/65 | 110/65 – 140/90 |