The first step in your assessment should be to get a general sense of the EKG. Mentally note if you see something out of the ordinary and come back to it as you go through your assessment. Do all the leads look normal?
Is there normal R-wave progression? Is AVR inverted? Be very general in this first assessment.
The second step begins our formal analysis of the 12-lead EKG. Check the calibration block on the 12-lead. Is it standard, half-standard, or 2 times standard? Don’t forget to do this.
The third step is to get the heart rate (ventricular and note the atrial rate). Determine if the rhythm is regular or irregular in general. Count the rate using the appropriate method for the rhythm (i.e., the 6 second method if the rhythm is irregular and the R to R method for a precise heart rate).
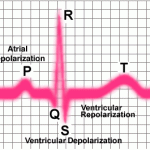
The fourth step is to specifically identify what rhythm is present on the EKG. Generally, start with p waves. Are they present? Do they all look the same? What is their rate? Are they regular? Most importantly, are each p wave associated with a QRS complex on the EKG? What is the PR interval? Next, look at the QRS. Is it narrow or wide? Ask yourself again, do they occur at regular or irregular intervals? If irregular, is the rhythm regularly irregular or irregularly irregular? This last step should be the final clue as to what the rhythm is.
The fifth step in our assessment is to determine what the mean QRS axis is. First, determine if Leads I and AVF are mostly positive, mostly negative, or biphasic to determine your quadrant. Next, find your most biphasic limb lead. Now, determine what lead is perpendicular to that biphasic lead and you have your axis vector. Remember to report the axis and the degrees of the vector, in that order.
The next step in our assessment is to check for signs of atrial enlargement or ventricular hypertrophy. Remember not to use enlargement and hypertrophy interchangeably, they are specific to atrial or ventricular. Also, it can be difficult at first to remember the guidelines for hypertrophy, so practice memorizing these guidelines whenever you can!
Atrial enlargement: First, take another scan of p-waves in each lead, but pay most attention to the p-waves in Lead II and V1 (best leads to look in for p-waves!). In Lead II, are the p-waves greater than 2.5 mm in height with a peaked look to them? If they do, you may have right atrial enlargement. Do the p-waves have a double peak and are greater than .11 sec in duration? If so, you may have left atrial enlargement. Next, look at p-waves in V1. Normally, V1 has an equiphasic look to it. If the first, upright portion of the p-wave is greater than 1 mm in height and width, and much larger than the downward portion, you may have right atrial enlargement. The opposite is true for left atrial enlargement (downward portion is larger than upright portion of p-wave).
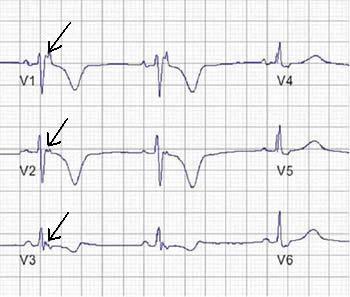
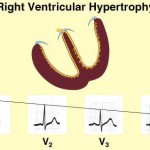 Ventricular hypertrophy: The next step is to look at the QRS complexes in V1-V6. If you have a reversal in R-wave progression and right axis deviation, then you may be looking at right ventricular hypertrophy. What seals the deal here is to also look at the QRS in V1, and if the height of the R wave is equal to or greater than the depth of the S wave, you have right ventricular hypertrophy. The last step is to evaluate the EKG for left ventricular hypertrophy. This is more tricky than the other abnormalities. There are three general guidelines to diagnose left ventricular hypertrophy: R wave height in AVL > 11 mm, R wave height in Lead I plus the S wave depth in Lead III that exceeds 25 mm, and, the most common, S wave depth in V1 plus the height in V5 that exceeds 35 mm. If you see one of these, you may have left ventricular hypertrophy. You may also see left axis deviation, but it is not needed for diagnosis. However, right axis deviation is needed for diagnosing right ventricular hypertrophy.
Ventricular hypertrophy: The next step is to look at the QRS complexes in V1-V6. If you have a reversal in R-wave progression and right axis deviation, then you may be looking at right ventricular hypertrophy. What seals the deal here is to also look at the QRS in V1, and if the height of the R wave is equal to or greater than the depth of the S wave, you have right ventricular hypertrophy. The last step is to evaluate the EKG for left ventricular hypertrophy. This is more tricky than the other abnormalities. There are three general guidelines to diagnose left ventricular hypertrophy: R wave height in AVL > 11 mm, R wave height in Lead I plus the S wave depth in Lead III that exceeds 25 mm, and, the most common, S wave depth in V1 plus the height in V5 that exceeds 35 mm. If you see one of these, you may have left ventricular hypertrophy. You may also see left axis deviation, but it is not needed for diagnosis. However, right axis deviation is needed for diagnosing right ventricular hypertrophy.
The seventh step in our 12 lead checklist deals with diagnosing bundle branch blocks. Diagnosing both kinds of blocks requires looking in the same leads; however, the QRS will look much different between the two blocks. But, the QRS complex, for both blocks, has to exceed a duration of greater than or equal to .12 sec.
Right bundle branch block: The leads to look in first for right bundle branch block (RBBB for short) are leads V1 & V2. In RBBB, the QRS complex has two R-waves which give the QRS a double-peaked appearance. This is called the “R-S-R1†wave. This must be present for RBBB. Next, to give further support to your diagnosis, look in leads I, V5, & V6. A good sign of RBBB is if the S wave has a “slurred†appearance or the end of the wave doesn’t return sharply back up to baseline.
Left bundle branch block: The leads to look in first for left bundle branch block (LBBB) are leads V5, V6, and I. If the QRS is wide, mostly upright, and the T waves are inverted, then you are most likely looking at LBBB. Next, to give further support to your diagnosis, look in leads V1-V3. If the QRS complexes are mostly negative (like big Q waves) and the T waves are upright, then you are for sure looking at LBBB.
The last step in our 12 lead EKG checklist is to diagnose myocardial infarction (MI). First, you need to remember what constitutes a “significant†Q wave. A significant Q wave is a wave that is at least 1 mm wide and greater than 1/3 the height of the R wave. Also, remember that a significant amount of ST segment elevation is an ST segment that is elevated by 1 mm or greater. Lastly, familiarize yourself again with the areas of the heart that each lead is looking at, this will help you immensely! I start my diagnosis by looking for lateral, inferior, and anterior MI’s, in that order.
Lateral MI: The leads to look in for lateral MI are leads I, AVL, V5, & V6. A significant Q wave in leads I & AVL is called an “old high lateral MIâ€, whereas ST segment elevation in these leads is called an “acute high lateral MIâ€. V5 & V6 look at the “low†lateral surface, so Q waves or ST segment elevation in these leads show old and acute “low lateral MI’sâ€.
Inferior MI: The leads to look in next are leads II, III, & AVF. Look for Q waves and ST elevation.
Anterior MI: Look at leads V1-V4 for anterior MI’s. Careful, do not overdiagnose the ST segments in V1 & V2. They are often normally elevated somewhat!
Posterior MI: This one is tricky, and the EKG is not the definitive diagnostic tool for this type of MI. But, look in V1 & V2 for tall R waves that will not be accompanied by right axis deviation. This is often confused with right ventricular hypertrophy. Careful with this one!!
If you follow these guidelines, you will be highly successful in correctly diagnosing abnormalities on the 12 lead EKG. Remember, take your time, follow the checklist carefully, and practice. As an objective detective, diagnosing a 12 lead EKG is like putting a puzzle together, just have fun while you’re at it!