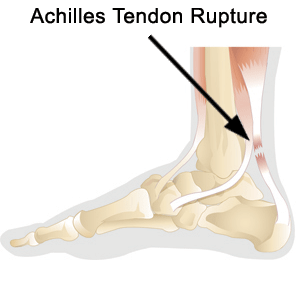
Specific steps to minimize the risk of Achilles tendon injury include:
- Wear the right shoes and sports shoes. The way a person walks, runs, and jumps is related to their individual bio-mechanics: their bone, muscle, and tendon structure. Achilles tendon injuries can be caused by common bio-mechanical issues such as high arches, low arches, having legs of slightly different lengths, etc. Bio-mechanical issues can often be addressed by wearing the right shoes.
- Warm up before stretching or exercising. The term “warm up†should be taken literally: exercise muscles a little to heat them up just prior to stretching or exercise. Spend a minimum of ten minutes warming up. Warm up examples include: walking slowly at the beginning of a long or fast walk, slow cross court movements and volleys prior to playing tennis, a brisk walk before jogging, jogging before running, lifting lighter weights before lifting weights, etc. Focus on the leg muscles, with particular attention to the calf muscles.
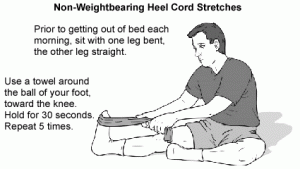 Stretch between warming up and exercising, and then again after exercising. Although there is some controversy about the value of stretching, many professionals believe that stretching helps prevent injury and that flexibility is a key component of fitness. Stretch the back, hip, thigh, and calf muscles. Tightness in one can lead to undue strain and tightness on the others.Pay particular attention to stretching the calf muscles because they are directly connected to the Achilles tendon. Stretching can be done lying down, sitting, or standing, and without any equipment.However, some stretches are easier to do with an elastic band pull, when leaning against a wall or on an inclined surface. Stretches are usually named after the muscle being stretched, i.e., gastroc (gastrocnemius) stretches and soleus stretches for the calf muscles. Stretch gently and slowly. Hold each stretch for half a minute to a minute.
Stretch between warming up and exercising, and then again after exercising. Although there is some controversy about the value of stretching, many professionals believe that stretching helps prevent injury and that flexibility is a key component of fitness. Stretch the back, hip, thigh, and calf muscles. Tightness in one can lead to undue strain and tightness on the others.Pay particular attention to stretching the calf muscles because they are directly connected to the Achilles tendon. Stretching can be done lying down, sitting, or standing, and without any equipment.However, some stretches are easier to do with an elastic band pull, when leaning against a wall or on an inclined surface. Stretches are usually named after the muscle being stretched, i.e., gastroc (gastrocnemius) stretches and soleus stretches for the calf muscles. Stretch gently and slowly. Hold each stretch for half a minute to a minute.
As part of a stretching program, also consider massage. Lightly massage the calf muscles before exercising and massage the calf muscles and Achilles tendons after exercising. Although there is some controversy as to the benefits of massage, many health professionals believe that massage: reduces muscle and tendon tightness, promotes healing, reduces the time muscles need to recover from exercise, and increases flexibility. Use the fingers to massage the Achilles tendons. Use a rolling pin (or similar commercial device) for the calf muscles. Apply ice therapy after massaging the Achilles tendons.
 Flexibility is difficult for many people to achieve: it often takes weeks or months of consistent stretching to achieve greater flexibility. For the best results: read some exercise books, consult with a trainer at your gym, or consult with a physical therapist.
Flexibility is difficult for many people to achieve: it often takes weeks or months of consistent stretching to achieve greater flexibility. For the best results: read some exercise books, consult with a trainer at your gym, or consult with a physical therapist.
- If you do aerobic and strengthening exercises on the same day, do the aerobic exercises first. In aerobic exercises, such as running or tennis, the leg muscles act as shock absorbers to protect the Achilles tendons, plus they work to keep the body aligned so that the Achilles tendons are not unduly twisted, stretched, or strained.  Strengthening exercises, such as weight lifting, are done to the point of muscle exhaustion. If strengthening exercises are done first, then the muscles will be too tired to do a good job protecting the Achilles tendons during the aerobic activity, increasing the chance of injury.
- Strengthen the leg muscles, particularly the calf muscles. Many people with Achilles injuries have disproportionately weak calf muscles. Leg exercises can be done without any equipment, with an elastic band pull, with free weights, or with exercise machines. Good leg strengthening exercises include: lunges, hip flexion band pulls, half (chair) squats, clean and press, leg press, inner and outer thigh band pulls, leg raises, leg extensions, and leg curls.
- Of particular benefit to the calf muscles, and therefore to the Achilles tendons, are calf raises and ankle band pulls. In order to help the Achilles tendon, focus on strengthening the eccentric (calf lowering) rather than concentric (calf raising) motion.
The anterior tibialis is the opposing muscle group to the calf muscles, so strengthening the anterior tibialis helps to stretch the calf muscles. The anterior tibialis is the small muscle group on the front of the lower leg: just to the right of the right leg’s shin bone and just to the left of the left leg’s shin bone. Its primary function is to flex the foot upward.
All of these exercises can be done in a variety of ways. For example, calf raises can be done with one or two legs using: standing or sitting calf raise machines, various leg press machines, a stool, a block of wood, a stairway, or on a curb.
 If the exercises are done consistently and properly, muscle strength will improve in as little as two weeks. Proceed consistently and gradually. For the best results: read some exercise books, consult with a trainer at your gym, or consult with a physical therapist.
If the exercises are done consistently and properly, muscle strength will improve in as little as two weeks. Proceed consistently and gradually. For the best results: read some exercise books, consult with a trainer at your gym, or consult with a physical therapist.
- Test for injuries after working out. Using the thumb and forefinger, lightly pinch different spots up and down the Achilles tendons. If the Achilles tendons are not sore, great. If they are sore, this may be an indication of Achilles tendinosis, which should be addressed right away.