Degenerative Joint Diseases
 A degenerative joint disease is the degeneration due to the “wear and tear†of joint surface cartilage that is usually accompanied by an overgrowth of bone, narrowing of joint spaces, hardening of bone on joint surface, and bone deformation. Osteoarthritisis a very common degenerative joint disease. Other types of arthritis like rheumatoid arthritis and post-traumatic arthritis and other inflammatory joint usually leads to osteoarthritis. Over many years of activity and use of joint, the “wear and tear†occurs and what happens is the cartilage surrounding the joint may become injured, torn, or worn out. When this protective cartilage is worn out, the surface of the bone on the affected side of the bone tends to rub and glide on the opposite surface of the bone, creating friction and eventually, damage the surrounding tissues and cause hardening of the joint surface. Pain, tenderness, swelling, and inflammation results and can greatly affect the daily activities of the person. A crepitus or cracking sound may be heard when moving the joint. It is called a degenerative disease since it will lead to a progressive deformity and may cause other co-morbidities and complications. This can be managed with physical therapy to strengthen the surrounding muscles, maintaining ideal body weights, and pain management with NSAIDs. If all these fails and depending on the severity of the disease, surgery may be the option.
A degenerative joint disease is the degeneration due to the “wear and tear†of joint surface cartilage that is usually accompanied by an overgrowth of bone, narrowing of joint spaces, hardening of bone on joint surface, and bone deformation. Osteoarthritisis a very common degenerative joint disease. Other types of arthritis like rheumatoid arthritis and post-traumatic arthritis and other inflammatory joint usually leads to osteoarthritis. Over many years of activity and use of joint, the “wear and tear†occurs and what happens is the cartilage surrounding the joint may become injured, torn, or worn out. When this protective cartilage is worn out, the surface of the bone on the affected side of the bone tends to rub and glide on the opposite surface of the bone, creating friction and eventually, damage the surrounding tissues and cause hardening of the joint surface. Pain, tenderness, swelling, and inflammation results and can greatly affect the daily activities of the person. A crepitus or cracking sound may be heard when moving the joint. It is called a degenerative disease since it will lead to a progressive deformity and may cause other co-morbidities and complications. This can be managed with physical therapy to strengthen the surrounding muscles, maintaining ideal body weights, and pain management with NSAIDs. If all these fails and depending on the severity of the disease, surgery may be the option.
Total Hip Replacement
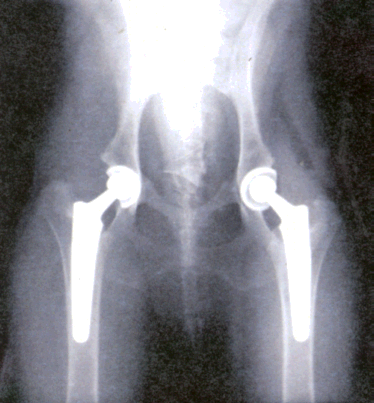
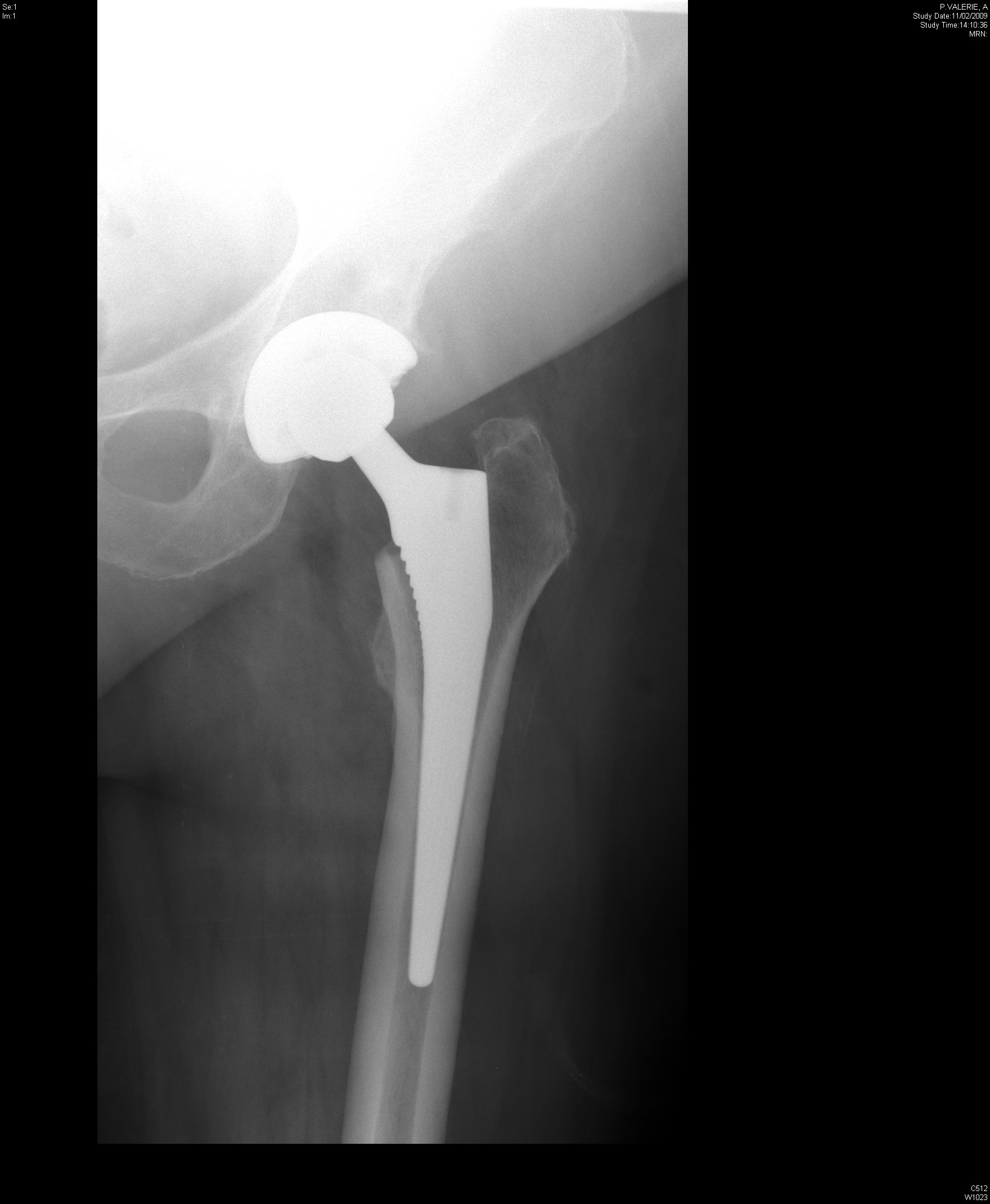
 Total hip replacement surgery have greatly reduced the number of arthoplasty procedures, especially in adults 50 years of age and above with degenerative joint disease of the hip. The goals of the surgery is for pain relief and to enable the person to return to his activities of daily living. In this surgery, the ball and socket of the hip are replaced. A small incision, about 10 centimeters long on the lateral aspect of the thigh to expose the femoral head. The femur is now dislocated from the acetabulum then a metal head on a metallic stem prosthesis, usually a titanium, is seated into the medullary canal of the femur. An acetabular cup component is configured on the acetabulum for articulation. This surgery is indicated for osteoarthritis, rheumatoid arthritis and other degenerative joint diseases. It is also sometimes indicated to repair disorders and fractures of the hip.
Total hip replacement surgery have greatly reduced the number of arthoplasty procedures, especially in adults 50 years of age and above with degenerative joint disease of the hip. The goals of the surgery is for pain relief and to enable the person to return to his activities of daily living. In this surgery, the ball and socket of the hip are replaced. A small incision, about 10 centimeters long on the lateral aspect of the thigh to expose the femoral head. The femur is now dislocated from the acetabulum then a metal head on a metallic stem prosthesis, usually a titanium, is seated into the medullary canal of the femur. An acetabular cup component is configured on the acetabulum for articulation. This surgery is indicated for osteoarthritis, rheumatoid arthritis and other degenerative joint diseases. It is also sometimes indicated to repair disorders and fractures of the hip.
Complications of total hip replacement
- Dislocation – This involves the dislocation of the prosthetic femoral head out of the replaced socket. Prior to hip surgery, the person’s hip has a ligament that links the ball of the joint into the socket. Naturally, there is also a think, dense tissue that surrounds the ball and socket to hold the articulation in place. During a total hip replacement surgery, these ligament and structures are removed. After surgery, there is no mechanical linking of the replaced ball into the socket. Only appropriate positioning of components within the patient and by muscles and ligaments that cross from the pelvis to the thigh holds it in place. This is the main reason why proper positioning is very imperative during the early post-operative phase. The patient should maintain abduction of the legs and must not bend the knee up to a 90 degree angle to prevent dislocation of prosthesis.
- Bleeding –Just like in any surgery, bleeding is a common risk. In the post-operative phase, bleeding may occur in the first and second days. Normally, a hemovac or asepto drain will be placed by the surgeon to collect the blood and avoid it from pooling in the operative site. Complete blood count is usually ordered post-operatively to know if the patient’s hemoglobin and hematocrit levels are in normal values. If these values go lower, iron supplements are advised to the person to increase blood counts. For severe bleeding, a blood transfusion may be necessary to prevent or restore blood levels.
- Debutius Ulcers – A patient who is immobile and requires complete bed rest is always at risk for developing pressure ulcers. Physical therapy is a must after a few days or weeks to ensure that the person practices range motion exercises and allow the person to ambulate at an earlier time to reduce risk of developing decubitus ulcers from prolonged bed rest and immobility.
- Infection – As with any surgery, infection should be prevented for a successful surgical management. Probable signs and symptoms of infection should be noted. Prior to surgery and postoperatively, the surgeon will load antibiotics to prevent infection.
- Wearing off of the Prosthesis – Since these prosthesis are made from artificial materials and over time, these components may also experience “wear and tear†just as with a natural hip joint.